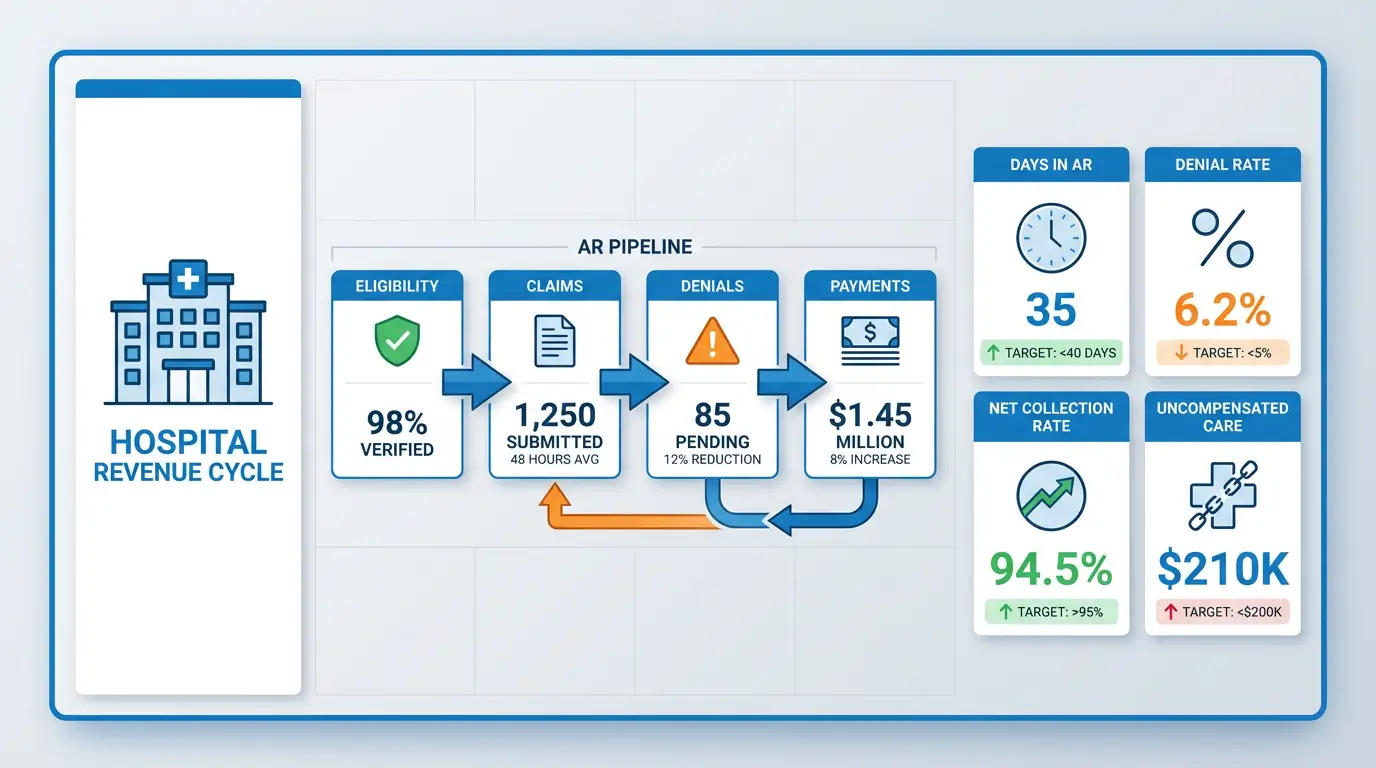
Introduction
Hospital accounts receivable management has become one of the most critical challenges facing healthcare operations today. According to recent industry data, hospitals lose an average of 4.2 million dollars annually to uncompensated care, and many struggle with accounts receivable aging that directly impacts cash flow and operational stability. For hospital operations managers, improving accounts receivable isn’t just about financial metrics—it’s about ensuring your organization has the resources to deliver quality patient care and invest in critical infrastructure.
The good news is that proven strategies exist to significantly improve your hospital’s accounts receivable performance. By combining improved medical billing processes, proactive patient coverage enrollment, and innovative technology solutions, you can reduce days in accounts receivable, minimize bad debt, and convert potential write-offs into actual revenue. This article explores the most effective approaches to strengthen your hospital’s AR management and boost your bottom line.
What Impacts Hospital Accounts Receivable Performance
Before implementing improvements, it’s essential to understand the key factors that affect your accounts receivable. Several interconnected elements influence how quickly you collect payment and how much revenue you ultimately recover.
Eligibility Verification and Patient Coverage
One of the largest contributors to AR problems is uninsured or underinsured patients. When patients arrive without active coverage, your billing team faces significant challenges in collecting payment. Many of these patients actually qualify for coverage options like Medicaid, Medicare, or ACA plans, but without proactive screening and enrollment, these opportunities are missed. This results in accounts that become increasingly difficult to collect as time passes.
Billing Process Efficiency
Inefficient billing workflows create delays that compound AR problems. When claims aren’t submitted promptly, denials aren’t addressed quickly, or documentation is incomplete, accounts age rapidly. Industry benchmarks show that hospitals with standardized, automated billing processes achieve significantly better collection rates than those relying on manual workflows.
Denial Management and Appeals
Claim denials represent lost revenue that many hospitals fail to recover. Without a systematic approach to analyzing denial patterns and submitting timely appeals, thousands of dollars slip away each month. The longer a denial sits unaddressed, the harder it becomes to appeal successfully.
Patient Communication and Payment Options
Patients with high deductibles or out of pocket costs often struggle to pay their balances. Without clear communication about payment options, flexible payment plans, and upfront cost estimates, patient collections suffer. Many hospitals miss opportunities to collect patient responsibility amounts because they don’t offer convenient payment methods or clear billing information.
How Improved Medical Billing Processes Strengthen Accounts Receivable
Implementing standardized, efficient medical billing processes is foundational to improving accounts receivable. These improvements directly reduce days in accounts receivable and accelerate cash flow.
Standardize Workflows and Documentation
The first step is documenting consistent billing and collection procedures across your organization. This includes standardized preregistration processes, eligibility verification workflows, and claim submission timelines. When every department follows the same procedures, you eliminate errors and financial leakage that occurs from inconsistent practices.
Leverage Automation and Technology
Modern billing technology dramatically improves AR performance. Robotic process automation (RPA) can handle eligibility verification, claims submission, and appeal letter generation with greater accuracy and speed than manual processes. Automation also reduces the administrative burden on your billing staff, allowing them to focus on complex accounts and denial analysis rather than repetitive data entry.
According to healthcare revenue cycle experts, hospitals implementing automation see measurable improvements in their net collection rates, with many achieving collection percentages above 95 percent. Automation also reduces “Discharged Not Final Billed” accounts, which represent significant revenue leakage.
Implement Real Time Analytics and Monitoring
You cannot improve what you don’t measure. Implementing real time analytics dashboards allows you to monitor critical KPIs including days in accounts receivable, denial rates, collection percentages, and aging account balances. Daily or weekly reviews of these metrics help you spot trends early and address problems before they become entrenched.
Establish Denial Analysis Teams
Denials represent one of the largest opportunities for AR improvement. Form a dedicated team to analyze denial patterns, identify root causes, and develop targeted solutions. Many hospitals discover that a small percentage of denials account for the majority of lost revenue. By focusing on these high impact denials, you can recover significant amounts quickly.
Why Getting Patients Approved for Medicaid Matters for Accounts Receivable
Medicaid enrollment represents one of the most powerful levers for improving hospital accounts receivable. Many uninsured patients who arrive at your hospital actually qualify for Medicaid coverage, but without proactive screening and enrollment support, this opportunity is lost.
The Financial Impact of Medicaid Enrollment
When an uninsured patient is successfully enrolled in Medicaid, your hospital transforms a potential write off into a billable, reimbursed claim. This conversion directly improves your accounts receivable by reducing uncompensated care and bad debt. Hospitals that prioritize Medicaid enrollment see measurable reductions in charity care write offs and faster overall collections.
Understanding the Medicaid Approval Timeline
Federal law requires states to approve or deny Medicaid applications within 45 days, or 90 days for applications requiring disability determinations. However, the actual timeline from initial application to final approval often extends beyond these minimums. Understanding these timelines helps you plan your billing strategy and set appropriate expectations for when claims can be submitted.
Hospital Role in Supporting Medicaid Enrollment
Your hospital can play an active role in helping patients navigate the Medicaid enrollment process. This includes assisting with application submission, gathering required documentation, and requesting expedited processing when medically necessary. By removing barriers to enrollment, you increase the percentage of patients who successfully obtain coverage.
Many states allow hospitals to submit full Medicaid applications on behalf of patients, streamlining the process and improving approval rates. This proactive approach converts more uninsured patients into covered patients, directly strengthening your accounts receivable.
Reducing Uncompensated Care Through Coverage Conversion
The relationship between Medicaid enrollment and uncompensated care is direct and measurable. Each patient successfully enrolled in Medicaid reduces your hospital’s uncompensated care burden. Over time, these individual conversions add up to significant financial impact on your bottom line and your accounts receivable aging.
How MyCareCoverage Helps Improve Accounts Receivable for Hospitals
MyCareCoverage is a digital platform designed specifically to help hospitals identify uninsured patients, screen them for coverage options, and facilitate enrollment to convert potential write offs into reimbursed claims.
Identifying and Screening Uninsured Patients
MyCareCoverage detects uninsured patients at or before the point of care and screens them for major coverage pathways including Medicaid, ACA plans, and Medicare. The platform also identifies patients who may qualify for ACA enrollment outside standard open enrollment periods through Qualifying Life Events, expanding coverage opportunities beyond traditional windows.
Streamlined Digital Enrollment Process
Rather than requiring patients to navigate complex enrollment processes independently, MyCareCoverage provides a user friendly digital platform. Patients access the system via personalized URL, self screen for coverage options, upload required documents in real time, and receive support from RevOne Patient Advocates when needed. This integration with your hospital’s financial assistance workflows ensures seamless coordination between patient enrollment and billing operations.
Automation That Reduces Staff Burden
The platform automates documentation, follow up communications, and returns eligibility and plan details directly to your billing team. This automation dramatically reduces the administrative burden on your staff while improving accuracy and speed. Your billing team receives the information they need to submit claims promptly, accelerating collections.
Proven Financial Results
Hospitals using MyCareCoverage report significant financial improvements. The platform delivers 3 to 5 times return on investment per converted uninsured case, transforming write offs into revenue. Many hospitals report that claims submitted for newly enrolled patients result in zero patient responsibility, meaning your hospital receives full reimbursement without patient collection challenges.
Beyond the direct revenue from converted cases, hospitals using MyCareCoverage see reductions in bad debt, uncompensated care, and charity write offs. The platform also improves cash flow, staff efficiency, and patient satisfaction by minimizing billing dead ends and front end delays that frustrate both patients and staff.
Key Performance Indicators to Monitor for Accounts Receivable Improvement
To ensure your AR improvement initiatives are working, you must track the right metrics. These KPIs provide visibility into your performance and help you identify areas needing additional attention.
Days in Accounts Receivable (DAR)
Days in accounts receivable measures the average number of days between service delivery and payment receipt. Lower DAR indicates faster collections and better cash flow. Industry benchmarks suggest targeting a DAR that reflects your payer mix, but most hospitals aim for continuous improvement in this metric.
Net Collection Rate
Your net collection rate measures the percentage of billable charges you actually collect. Hospitals with net collection rates below 95 percent have significant opportunity for improvement through better processes and technology. Tracking this metric helps you understand your overall collection effectiveness.
Denial Rate and Denial Recovery Rate
Monitor both the percentage of claims denied and your success rate in appealing denials. High denial rates indicate problems in coding, documentation, or claims submission that need addressing. Your denial recovery rate shows what percentage of denied claims you successfully appeal and collect.
Accounts Receivable Aging
Track the percentage of your AR that falls into aging categories: 0 30 days, 31 60 days, 61 90 days, 91 180 days, and over 180 days. Accounts that age beyond 90 days become increasingly difficult to collect. Monitoring aging helps you allocate collection resources effectively and identify systemic problems.
Uncompensated Care and Bad Debt
These metrics directly reflect your success in identifying and enrolling uninsured patients in coverage. Reductions in uncompensated care and bad debt indicate that your Medicaid enrollment and coverage conversion efforts are working.
Conclusion
Improving hospital accounts receivable requires a multifaceted approach that addresses billing process efficiency, patient coverage enrollment, and strategic use of technology. By standardizing your billing workflows, implementing automation, prioritizing Medicaid enrollment, and leveraging solutions like MyCareCoverage, you can significantly reduce your days in accounts receivable and convert potential write offs into actual revenue.
The financial impact of these improvements extends beyond accounts receivable metrics. Better AR management means improved cash flow, reduced bad debt, lower uncompensated care, and greater financial stability for your organization. For hospital operations managers, these improvements translate into resources available for patient care, staff development, and facility improvements.
Start by assessing your current AR performance against industry benchmarks. Identify your biggest opportunities for improvement, whether that’s process standardization, technology implementation, or enhanced patient coverage enrollment. Then implement changes systematically, monitor your KPIs closely, and adjust your approach based on results. With commitment to continuous improvement, your hospital can achieve significant gains in accounts receivable performance and financial health.