Introduction

The expansion of Medicaid over the past decade has fundamentally transformed hospital financial performance. Following the Affordable Care Act’s Medicaid expansion, hospitals saw an average decrease of $2.8 million in uncompensated care costs, representing a significant improvement in financial stability and operational efficiency. However, a major regulatory change is coming that threatens to reverse these gains and create substantial financial challenges for healthcare systems across the country.
Starting January 1, 2027, the One Big Beautiful Bill Act (OBBBA) will require states to conduct Medicaid eligibility redeterminations every six months for the expansion population, up from the current annual requirement. This shift from annual to semi annual redeterminations represents a fundamental change in how Medicaid coverage is managed and will have profound implications for hospital revenue, patient care, and financial planning. The increased frequency of redeterminations means more opportunities for patients to lose coverage, and many hospitals are unprepared for the financial impact.
The challenge is significant: an estimated 10 to 15 million people from the Medicaid expansion population are expected to lose coverage due to income threshold changes and administrative barriers. For hospital executives, understanding Medicaid redetermination requirements and preparing proactive strategies is no longer optional—it is essential to maintaining financial stability and ensuring continuity of care for vulnerable patient populations.
What Is the One Big Beautiful Bill Act and Why Does It Matter for Hospitals?

The One Big Beautiful Bill Act represents a significant shift in Medicaid policy that will reshape how states manage eligibility and coverage. Effective January 1, 2027, the OBBBA requires states to conduct Medicaid eligibility redeterminations every six months for the expansion population (adults aged 19 to 64 who became eligible under the ACA Medicaid expansion). This is a dramatic change from the current annual redetermination schedule.
Key provisions of the OBBBA that affect hospitals include:
- Semi annual redeterminations for expansion population: States must redetermine eligibility every six months instead of annually
- Continued annual renewals for exempt groups: Children, pregnant women, and disabled individuals continue with annual redetermination schedules
- Retroactive coverage reduction: For the expansion population, retroactive coverage will be reduced from 90 days to 30 days, meaning patients who lose coverage will have less time to address coverage gaps
- Implementation timeline: All changes take effect January 1, 2027, giving hospitals less than two years to prepare
The rationale behind these changes centers on ensuring that Medicaid coverage is limited to those who remain eligible based on current income and circumstances. However, the practical effect is that more frequent redeterminations create more opportunities for coverage loss, particularly among patients whose income fluctuates or who struggle with administrative requirements.
For hospital executives, the OBBBA represents a critical inflection point. The financial models that have guided hospital planning for the past decade will need to be recalibrated to account for increased uncompensated care, higher bad debt expenses, and greater administrative burden on patient access services.
How Will Semi Annual Redeterminations Impact Hospital Patient Coverage?
The shift to semi annual Medicaid redeterminations will have cascading effects throughout hospital operations and financial performance. More frequent redeterminations create exponentially more opportunities for coverage loss, administrative errors, and gaps in patient insurance status.
The Coverage Loss Mechanism
With semi annual redeterminations, patients must verify their eligibility twice per year instead of once. This doubled frequency means:
- Patients must provide updated income documentation twice annually
- Administrative errors or missed deadlines result in coverage loss twice as often
- Income fluctuations that might have been absorbed in an annual cycle now trigger coverage loss
- Patients working seasonal or variable income jobs face heightened risk of coverage gaps
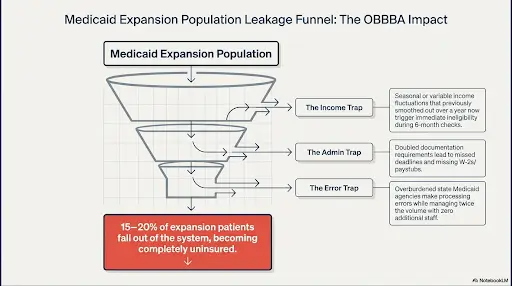
Expected Coverage Loss Volume
Research from the Urban Institute and Kaiser Family Foundation indicates that 10 to 15 million people from the Medicaid expansion population will lose coverage as a result of the OBBBA requirements. This represents approximately 15 to 20 percent of the expansion population. For a typical hospital system serving a population with significant Medicaid enrollment, this could translate to thousands of patients losing coverage annually.
Disproportionate Impact on Vulnerable Hospitals
The impact of semi annual Medicaid redeterminations will not be evenly distributed across all hospitals. Safety net hospitals and rural hospitals will face the most severe financial consequences:
- Safety net hospitals: These institutions serve disproportionately high percentages of Medicaid and uninsured patients. A 15 to 20 percent reduction in Medicaid coverage among their patient population could result in millions of dollars in additional uncompensated care costs
- Rural hospitals: Many rural hospitals operate on thin margins and depend heavily on Medicaid reimbursement. The loss of Medicaid coverage for significant portions of their patient base could threaten financial viability
- Hospitals in non expansion states: While these hospitals have not benefited from Medicaid expansion, they may face increased patient migration and referral patterns as coverage changes
Administrative Burden
Beyond the direct financial impact, semi annual redeterminations create substantial administrative burden for both states and hospitals. State Medicaid agencies must process twice as many redeterminations with existing staffing and resources. Hospitals must:
- Verify patient insurance status more frequently
- Update billing systems and claims processing procedures
- Manage more coverage gaps and denials
- Increase patient outreach and education efforts
- Expand financial counseling and patient access services
What Happens When Patients Lose Medicaid Coverage?
Understanding the mechanics of coverage loss is essential for hospital executives developing response strategies. When a patient loses Medicaid coverage due to redetermination, a specific sequence of events occurs that creates both challenges and opportunities for hospitals.
The Coverage Loss Process
When a patient fails to complete redetermination or no longer meets income eligibility requirements, their Medicaid coverage terminates. States are required to provide advance notice of redetermination requirements and coverage termination, typically 30 to 60 days before coverage ends. However, many patients do not understand these notices or fail to take action, resulting in unexpected coverage loss.
Qualifying Life Events and ACA Marketplace Access
A critical but often overlooked fact is that loss of Medicaid coverage constitutes a Qualifying Life Event (QLE) under the Affordable Care Act. This means that patients who lose Medicaid coverage are eligible to enroll in ACA Marketplace plans outside of the standard open enrollment period. Specifically:
- Patients have 60 days from the date of Medicaid coverage loss to enroll in an ACA Marketplace plan
- This special enrollment period allows patients to access subsidized coverage based on their current income
- Many patients who lose Medicaid coverage will qualify for substantial ACA subsidies, making Marketplace coverage affordable
Coverage Gaps and Financial Impact
Despite the availability of ACA Marketplace coverage, significant gaps often occur between Medicaid loss and Marketplace enrollment:
- Patients may not be aware of their QLE or the special enrollment period
- Administrative delays in Medicaid termination and Marketplace enrollment create gaps
- Patients may delay enrollment, hoping to regain Medicaid eligibility
- Some patients may choose to remain uninsured rather than navigate the enrollment process
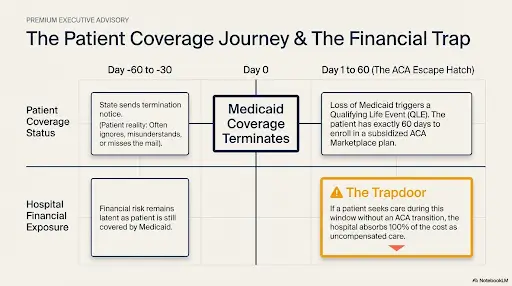
These coverage gaps create direct financial consequences for hospitals. When patients lose Medicaid coverage and do not immediately enroll in alternative coverage, hospitals must absorb the cost of care as uncompensated care. Unlike Medicaid reimbursement, which typically covers 70 to 90 percent of costs, uncompensated care generates zero revenue while consuming full resources.
Uncompensated Care Cost Escalation
The financial impact of coverage loss is substantial. National estimates suggest that if 10 to 15 million people lose Medicaid coverage as a result of the OBBBA, uncompensated care costs could increase by $18.9 billion nationally. For individual hospitals, the impact depends on their patient population and geographic location, but the financial pressure will be significant across the industry.
How Can Hospitals Help Patients Navigate Redetermination?
While the regulatory environment is changing, hospitals are not passive victims of these changes. Proactive patient engagement and support strategies can significantly mitigate the impact of semi annual Medicaid redeterminations. Hospital executives should prioritize patient engagement initiatives that help patients maintain coverage or transition smoothly to alternative coverage options.
Patient Education and Outreach
The foundation of effective redetermination management is patient education. Many patients do not understand Medicaid redetermination requirements or the consequences of missing deadlines. Hospitals should implement comprehensive patient education programs that:
- Explain Medicaid redetermination requirements and timelines
- Clarify income thresholds and what changes trigger redetermination
- Provide clear instructions for completing redetermination applications
- Explain the consequences of missing redetermination deadlines
- Outline alternative coverage options, including ACA Marketplace plans
Proactive Patient Identification
Hospitals should use their patient data and electronic health record systems to identify patients at risk of coverage loss. This includes:
- Patients approaching redetermination deadlines
- Patients with income near Medicaid eligibility thresholds
- Patients with history of coverage gaps or administrative issues
- Patients with seasonal or variable income patterns
Financial Counseling and Documentation Support
Many patients lose Medicaid coverage not because they are ineligible, but because they fail to provide required documentation or complete the redetermination process. Hospitals should expand financial counseling services to:
- Help patients gather required income documentation
- Assist with redetermination application completion
- Explain income verification requirements
- Provide guidance on what documentation is acceptable
- Follow up with patients to ensure timely submission
Timely Communication About Coverage Changes
When patients lose coverage, immediate communication is essential. Hospitals should:
- Notify patients of coverage loss as soon as it occurs
- Explain the Qualifying Life Event and special enrollment period
- Provide information about ACA Marketplace enrollment
- Offer assistance with Marketplace enrollment
- Discuss financial assistance programs and payment plans
What Role Can Technology Play in Managing Redetermination?
Technology solutions are essential tools for hospitals managing the complexity of semi annual Medicaid redeterminations. The right technology platform can streamline patient engagement, reduce coverage gaps, and minimize uncompensated care costs.
Patient Risk Identification and Alerts
Advanced analytics and data integration tools can identify patients at risk of coverage loss before it occurs. These systems can:
- Monitor patient income and eligibility status
- Generate alerts for upcoming redetermination deadlines
- Flag patients with income near eligibility thresholds
- Identify patients with history of coverage gaps
- Prioritize outreach efforts based on risk level
Automated Patient Communication
Technology platforms can automate patient communication about redetermination requirements and coverage changes:
- Automated reminders about redetermination deadlines
- SMS and email notifications about coverage status changes
- Patient portals with redetermination status and required actions
- Automated alerts when coverage is about to terminate
- Integration with patient communication systems for coordinated outreach
Seamless Enrollment into Alternative Coverage
When patients lose Medicaid coverage, technology can facilitate rapid enrollment into ACA Marketplace plans. Integrated enrollment platforms can:
- Automatically identify patients as eligible for special enrollment periods
- Pre populate Marketplace applications with patient data
- Streamline the enrollment process to reduce administrative burden
- Provide real time information about available plans and subsidies
- Track enrollment status and follow up with patients
Integrated Coverage Management Solutions
Comprehensive platforms like MyCareCoverage exemplify how technology can address the full spectrum of Medicaid redetermination challenges. These solutions help patients:
- Complete Medicaid redetermination applications
- Understand eligibility requirements and income thresholds
- Enroll in ACA Marketplace plans when Medicaid is lost
- Access subsidies and financial assistance
- Maintain continuous coverage throughout transitions
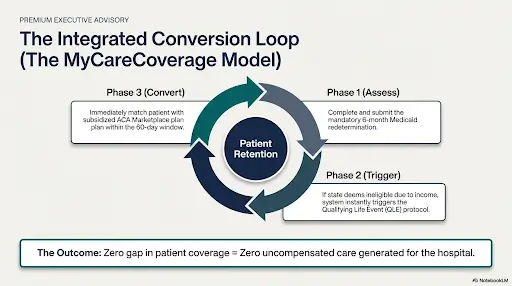
By integrating Medicaid redetermination and ACA Marketplace enrollment into a single platform, hospitals can significantly reduce coverage gaps and the resulting uncompensated care costs.
Data Integration and Reporting
Technology platforms should provide comprehensive reporting and analytics that help hospital executives:
- Track redetermination outcomes and coverage loss rates
- Monitor uncompensated care trends
- Measure the effectiveness of patient engagement initiatives
- Identify operational bottlenecks and improvement opportunities
- Forecast financial impact of coverage changes
What Financial Impact Should Hospitals Expect?
Hospital executives must understand the financial implications of semi annual Medicaid redeterminations to develop appropriate response strategies and budget forecasts. The financial impact will be substantial and multifaceted.
National Uncompensated Care Projections
If 10 to 15 million people lose Medicaid coverage as a result of the OBBBA, national uncompensated care costs could increase by $18.9 billion. This represents a significant reversal of the financial gains hospitals achieved through Medicaid expansion. For context, this $18.9 billion increase in uncompensated care costs exceeds the annual operating margin of most hospital systems.
Hospital Revenue Loss from Reduced Medicaid Payments
Beyond uncompensated care, hospitals will experience direct revenue loss from reduced Medicaid payments. When patients lose coverage:
- Medicaid reimbursement (typically 70 to 90 percent of costs) is replaced by uncompensated care (zero revenue)
- The difference between Medicaid reimbursement and uncompensated care represents direct revenue loss
- For a hospital with significant Medicaid volume, this can translate to millions of dollars in annual revenue loss
Disproportionate Impact on Safety Net and Rural Hospitals
The financial impact will not be evenly distributed. Safety net hospitals and rural hospitals will face the most severe consequences:
- Safety net hospitals serving predominantly Medicaid populations could see 15 to 20 percent reductions in Medicaid revenue
- Rural hospitals operating on thin margins may face financial viability challenges
- Hospitals in states with high Medicaid expansion enrollment will experience greater impact
Operational Cost Increases
Beyond revenue loss, hospitals will incur increased operational costs:
- Expanded patient access and financial counseling services
- Technology investments in redetermination management systems
- Increased bad debt write offs and collection costs
- Administrative costs for managing coverage gaps and denials
- Training and staffing for patient engagement initiatives
Planning and Preparation as Financial Imperative
The financial impact of semi annual Medicaid redeterminations can be partially mitigated through proactive planning and preparation. Hospitals that invest in patient engagement, technology solutions, and operational improvements now will experience significantly lower financial impact than those that wait until 2027 to respond.
Conclusion
The shift to semi annual Medicaid redeterminations starting January 1, 2027, represents one of the most significant regulatory changes affecting hospital finances in the past decade. An estimated 10 to 15 million people will lose Medicaid coverage, potentially increasing national uncompensated care costs by $18.9 billion. For hospital executives, this is not a distant concern—it is an immediate imperative requiring strategic planning and operational preparation.
The good news is that hospitals are not powerless in the face of these changes. Proactive patient engagement, strategic use of technology, and comprehensive enrollment support can significantly mitigate the financial impact of coverage loss. Hospitals that help patients maintain Medicaid coverage or transition smoothly to ACA Marketplace plans will experience lower uncompensated care costs, better patient outcomes, and improved financial performance.
Now is the time to evaluate your patient engagement and enrollment strategies. Assess your current capabilities for identifying at risk patients, supporting redetermination applications, and facilitating enrollment into alternative coverage. Invest in technology solutions that streamline these processes and reduce coverage gaps. Expand financial counseling and patient access services to support patients through coverage transitions. The hospitals that take action today will be best positioned to navigate the challenges of semi annual Medicaid redeterminations and protect their financial stability in 2027 and beyond.

